Introduction
Surfer’s myelopathy is a rare but potentially serious condition that primarily affects surfers, especially beginners. Little known to the general public and often misdiagnosed, this neurological condition results from spinal cord compression due to prolonged hyperextension of the spine. Unlike acute trauma often associated with extreme sports, surfer’s myelopathy does not result from a direct impact, but rather from a posture maintained over a long period of time, leading to sometimes severe neurological disorders.
Although surfing is generally perceived as an accessible board sport that benefits physical well-being, it exposes surfers to specific mechanical constraints. When a surfer paddles to catch a wave, they adopt a posture of prolonged dorsal and cervical hyperextension, thus exerting constant pressure on the spinal cord. In some people, this can cause spinal cord ischemia, a temporary reduction in blood flow to the spinal cord, resulting in neurological symptoms ranging from simple numbness to partial or complete paralysis.
Understanding risks to better prevent them
One of the major challenges of surfer’s myelopathy is its delayed diagnosis. Initial symptoms, such as tingling in the legs, muscle weakness, or difficulty with coordination, are often attributed to fatigue or temporary cramps. However, in the most severe cases, this condition can progress to temporary paraplegia, requiring prompt treatment to avoid long-term complications.
Lack of awareness of this condition among both surfers and healthcare professionals contributes to delayed diagnosis. Many patients undergo multiple consultations before receiving an accurate diagnosis, which can compromise their recovery. Magnetic resonance imaging (MRI) remains the gold standard for detecting spinal cord injuries associated with this condition.
Prevention plays a key role in managing the risks associated with surfer’s myelopathy. Proper physical preparation, including muscle strengthening and flexibility exercises for the back and neck, can reduce the pressure placed on the spinal cord during surfing. Similarly, adopting optimized postural techniques and taking regular breaks during sessions can limit prolonged stress on the spine.
Finally, raising awareness among surfers, especially novices, about the warning signs of this condition is essential for early treatment. A better understanding of the risks and preventive solutions can help avoid serious complications and allow enthusiasts to fully enjoy their sport in complete safety.
In short, surfer’s myelopathy illustrates the importance of prevention and a thorough understanding of the physiological impacts of surfing on the body. While this condition remains rare, it serves as a reminder that even seemingly harmless sports can have significant medical consequences. Increased vigilance and appropriate postural adjustments are key to reducing risks and ensuring safer, more sustainable surfing.
Origin and Trigger of Surfer’s Myelopathy
Surfer’s myelopathy is a rare but serious condition resulting from specific mechanical stresses associated with surfing posture. This non-traumatic neurological condition primarily occurs in novice surfers, who spend extended periods paddling in a prone position with hyperextension of the back and neck. Although often underestimated, this prolonged position can cause spinal cord compression and sometimes severe neurological symptoms.
Surfing and mechanical constraints: a risky duo
Surfing, although often perceived as a fluid and harmonious water sport, places intense demands on the body, particularly the spine. When a surfer paddles to catch a wave, they maintain a prolonged position where their torso is elevated while their arms perform repetitive movements. This posture places significant stress on the lumbar and cervical regions.
In some people, this prolonged position causes a reduction in blood flow to the spinal cord, a phenomenon called spinal cord ischemia. This lack of blood flow leads to cellular damage that can result in numbness, muscle weakness, and, in extreme cases, loss of control of the lower limbs. The sudden onset of these symptoms can surprise practitioners, as they often occur without prior pain or clear warning signs.
Cervical Hyperextension: The Main Culprit
One of the main triggers of surfer’s myelopathy is excessive and prolonged hyperextension of the cervical spine. When the surfer raises their head while lying on the board, their cervical spine is subjected to significant pressure, which can affect blood circulation in the spinal cord. This position causes compression of vascular structures, particularly the anterior spinal arteries, which play a crucial role in oxygenating the spinal cord.
Additionally, cervical hyperextension can irritate nerve roots and promote compression of the intervertebral discs. This can not only cause local inflammation but also increase vulnerability to spinal cord injury. Repeated microtraumas can accelerate the degenerative process, increasing the risk of developing neurological symptoms.
Aggravating factors: posture, duration and intensity
Several factors can increase the risk of surfer’s myelopathy:
- Prolonged hyperextension : The longer a surfer lies on their board in a paddling position, the more pressure is placed on the spinal cord. Beginner surfers, who spend more time paddling without changing their position, are particularly at risk.
- Intensity and frequency of sessions : Prolonged sessions without adequate breaks increase the likelihood of spinal cord ischemia. Lack of recovery between sessions can exacerbate accumulated tension.
- Surfer’s Flexibility and Fitness : Inadequate back muscle conditioning or a lack of cervical and lumbar flexibility can increase the stress on the spine. People with muscle stiffness or a predisposition to spinal problems are at greater risk.
- Environment and water temperature : Cold can exacerbate vascular phenomena by reducing blood circulation, which can amplify the effects of spinal cord ischemia.
By understanding these mechanisms and adopting appropriate prevention strategies, surfers can reduce their risk of developing this pathology and preserve their spinal health in the long term.
Neurological Mechanisms and Dysfunctions
Surfer’s myelopathy is based on complex pathophysiological mechanisms that directly affect the spinal cord. This pathology, although non-traumatic, causes neurological lesions that can permanently alter the motor skills and sensitivity of the lower limbs. The origin of the disorder is mainly based on spinal cord compression , a progressive and often silent process, but also on vascular phenomena such as spinal ischemia , which aggravate neuronal suffering. These alterations disrupt nerve transmission , leading to variable motor and sensory deficits depending on the intensity of the damage.
Spinal cord compression: an insidious process
Spinal cord compression plays a central role in the development of surfer’s myelopathy. When a surfer adopts a prolonged position of hyperextension of the back and neck, the cervical spine experiences unusual mechanical stresses. These stresses exert excessive pressure on the vertebrae, intervertebral discs, and surrounding structures, progressively compressing the spinal cord.
This compression is often painless at first, which is why it goes unnoticed. However, over time, it disrupts the blood supply and oxygen supply to spinal cord neurons, leading to a progressive decline in their function. This can cause neurological symptoms such as tingling, muscle weakness, and, in the most severe cases, loss of control of the lower limbs.
If compression persists, it can lead to degenerative damage affecting the nerve bundles responsible for motor and sensory control. This insidious progression underscores the importance of early detection to avoid permanent damage.
Spinal ischemia and inflammatory response
Another key factor in the pathophysiology of surfer’s myelopathy is spinal ischemia , which is a decrease in blood flow to the spinal cord. This phenomenon results primarily from vascular compression induced by prolonged extension posture.
The spinal cord is supplied by a network of small arteries, including the anterior spinal artery , which plays a vital role in oxygenating neurons. When a surfer remains in hyperextension for too long, these vessels can become temporarily compressed, reducing the supply of oxygen and nutrients. This hypoxia causes cellular distress, which can rapidly impair neurological function and cause motor and sensory deficits.
In response to this ischemia, an inflammatory reaction can be triggered, further aggravating the situation. The inflammation causes localized edema, which increases spinal cord compression and promotes the degeneration of nerve tissue. This inflammatory process explains why some patients experience a progressive worsening of symptoms even after stopping activity.
Consequences on nerve transmission
Spinal cord neurons play a vital role in communication between the brain and the rest of the body. Any spinal cord injury therefore disrupts the transmission of nerve signals, affecting motor skills and sensation in the lower limbs.
In surfer’s myelopathy, damage to the spinal tracts can lead to:
- A loss of muscle strength , ranging from mild weakness to complete paralysis of the legs.
- An alteration of reflexes , sometimes with exaggerated responses or on the contrary a reduction in muscle reactivity.
- Sensitivity disturbances , such as numbness, tingling, or loss of tactile perception.
- Difficulties with coordination and balance , making walking unsteady and increasing the risk of falls.
- In the most severe cases, there is damage to autonomic functions , which can cause urinary or intestinal problems.
The severity of symptoms depends on the intensity and duration of spinal cord compression. Prompt diagnosis and treatment are essential to limit damage and promote nerve recovery.
Symptoms and Warning Signs
Surfer’s myelopathy presents with progressive neurological symptoms that can, in some cases, progress to severe spinal cord injury. This often insidious condition typically begins with mild sensory and motor disturbances but can rapidly worsen if spinal cord compression and ischemia persist. Early recognition of warning signs is essential to avoid long-term complications and enable appropriate management.
Numbness and loss of sensation: first signs
One of the first symptoms experienced by people with surfer’s myelopathy is numbness or tingling in the lower limbs. These abnormal sensations, often compared to pins and needles or electric shocks, are a sign of damage to the sensory pathways in the spinal cord.
These sensory disorders generally appear gradually after a prolonged surfing session and can affect:
- Feet and toes, giving a feeling of “numb feet” or loss of contact with the ground.
- The legs, causing difficulty feeling pressure, heat or cold.
- More rarely, the hands or arms in the case of extensive cervical involvement.
In some cases, surfers describe a feeling of stiffness or heaviness in their legs, making walking less fluid. Although these symptoms may disappear spontaneously after a few hours of rest, their persistence should prompt medical attention.
Muscle weakness and motor disorders
If spinal cord compression intensifies, motor difficulties appear. Patients begin to experience weakness in the legs, which may manifest as:
- A reduction in muscle strength , making it difficult to maintain balance or climb stairs.
- A feeling of heavy or soft legs , requiring frequent breaks when walking.
- A decrease in muscle reflexes , often detected during a neurological examination.
In more advanced cases, loss of motor control can cause coordination problems and unsteady walking . Some patients describe a sensation of dragging feet , as if they have difficulty lifting their legs properly. This development indicates deeper damage to the nerve pathways and requires rapid treatment to prevent worsening.
Persistent back and neck pain
Although surfer’s myelopathy is primarily a neurological condition, it can also be accompanied by spinal pain . This results from excessive strain on the cervical and dorsal vertebrae during prolonged prone paddling.
The most common pains are:
- Neck pain : A feeling of stiffness or burning in the neck, sometimes radiating to the shoulders or head.
- Back pain : Pressure in the middle of the back, which may be exacerbated by certain movements or prolonged postures.
- Postural headaches : Some people experience headaches related to accumulated tension in the cervical region.
These pains are usually muscular and postural , but they can mask an underlying spinal cord injury. If they are accompanied by neurological symptoms (numbness, muscle weakness), a thorough medical evaluation is essential.
Severe damage: when the spinal cord suffers
In the most severe forms, surfer’s myelopathy can develop into severe spinal cord damage , leading to major neurological deficits:
- Complete loss of sensation in the legs , which can lead to temporary paraplegia.
- Urinary or intestinal disorders , indicating damage to the autonomic functions of the spinal cord.
- Absence of tendon reflexes , a sign of advanced spinal nerve dysfunction.
- Altered muscle tone , with spasms or, on the contrary, significant hypotonia.
These symptoms, although rare, require emergency treatment to limit potential after-effects. Prompt treatment, including temporary immobilization and targeted medical interventions, can promote recovery and prevent irreversible damage.
Pathophysiology
The pathophysiology of surfer’s myelopathy lies in the repetitive mechanical stresses placed on the spine, particularly the neck and cervical spine, during surfing. These constant and specific movements associated with surfing, such as excessive neck flexion, rotation, and shock during falls, can lead to progressive alterations of the spinal cord.
Excessive neck flexion is a key component of the pathophysiology. While paddling, surfers frequently adopt a neck flexion position to paddle and maintain balance on the board. This repeated action, combined with impacts from falls or waves, exposes the spinal cord to considerable mechanical forces, resulting in repetitive strain injuries.
These mechanical stresses can cause compression of the intervertebral discs, herniated discs, and damage to the surrounding tissues. These structural alterations of the spine can lead to direct compression of the spinal cord, disrupting the normal transmission of nerve signals.
The resulting damage can affect the sensory and motor pathways of the spinal cord. Symptoms, such as numbness, tingling, muscle weakness, and coordination problems, reflect this disruption in nerve communication. Damage to nerve fibers can lead to decreased sensation and muscle strength, impacting the ability to perform precise and coordinated movements.
The pathophysiology of surfer’s myelopathy may also involve inflammatory processes in response to repetitive microtrauma. Inflammation can exacerbate injuries and contribute to the painful symptoms associated with the condition.
Medical imaging, particularly magnetic resonance imaging (MRI), is often used to visualize structural abnormalities of the spinal cord and confirm the diagnosis. A thorough clinical assessment, combined with radiological studies, is essential to understand the nature and extent of the damage, which then guides the appropriate management for each patient.
Comparison with Other Spinal Cord Disorders
Surfer’s myelopathy shares some characteristics with other spinal cord disorders, which can sometimes complicate its diagnosis. However, it is distinguished by its mechanism of onset, its non-traumatic nature, and its direct association with specific physical activity. Comparing this pathology with herniated discs, spinal stenosis, and traumatic myelopathies allows for a better understanding of its specificities and the adoption of more targeted management.
Herniated discs and spinal stenosis: deceptive similarities
Herniated disc and spinal stenosis are two well-known conditions that can cause spinal cord compression and neurological symptoms similar to those seen in surfer’s myelopathy.
- Herniated disc : This occurs when the nucleus of an intervertebral disc protrudes from its covering and compresses the spinal cord or nerve roots. This compression causes back pain, numbness, and muscle weakness, symptoms that can be reminiscent of surfer’s myelopathy. However, a herniated disc usually results from progressive degeneration or acute trauma , not from prolonged posture as in surfer’s myelopathy.
- Spinal stenosis : This is a narrowing of the spinal canal, often caused by osteoarthritis or degenerative changes in the spinal structures. Like surfer’s myelopathy, it can lead to chronic spinal cord compression , pain, and motor impairment. However, spinal stenosis progresses slowly with aging and primarily affects older adults , while surfer’s myelopathy often affects healthy young athletes.
A key distinction between these conditions and surfer’s myelopathy is the course of symptoms . Herniated discs and spinal stenosis develop gradually and worsen over time, whereas surfer’s myelopathy appears suddenly , often after a long surfing session.
Traumatic Myelopathy vs Surfer’s Myelopathy
Traumatic myelopathy is another spinal cord condition that shares similarities with surfer’s myelopathy, particularly in terms of motor and sensory deficits. However, these two conditions differ significantly in their mechanism of onset and clinical course .
- Traumatic myelopathy : This results from a violent impact or direct trauma to the spine, such as a vertebral fracture or dislocation. This injury causes immediate damage to the spinal cord, often accompanied by a sudden loss of motor skills and sensation.
- Surfer’s myelopathy : Unlike the traumatic form, it does not result from a direct shock , but from prolonged hyperextension of the cervical spine . The spinal cord suffers progressive compression and a lack of blood flow (ischemia), which leads to a deterioration of neurological functions without immediate physical injury.
One of the major differences between these two forms of myelopathy is the possibility of recovery . In surfer’s myelopathy, symptoms may improve with adequate rest and early rehabilitation, whereas in traumatic myelopathy, damage is often permanent due to destruction of nerve fibers.
Understanding the differences to better treat
Differentiating surfer’s myelopathy from other spinal cord disorders is essential for appropriate management. Here are some key criteria:
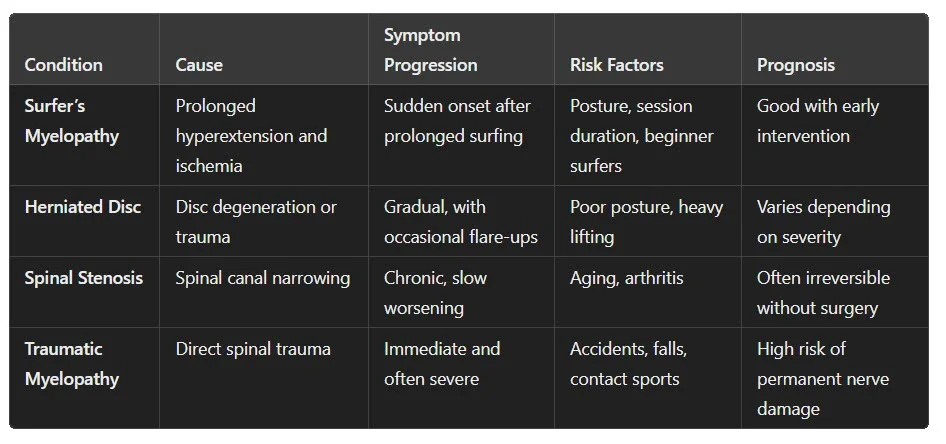
Differential diagnosis is based primarily on clinical examination , medical imaging (MRI) , and analysis of the patient’s history . In the case of surfer’s myelopathy, early management with rest, rehabilitation, and postural correction often results in satisfactory recovery.
This comparison highlights the importance of prevention and awareness to avoid complications and promote a safe return to normal activity.
The Impact of Surfing on Spinal Health
Surfing, although associated with a fluid and beneficial activity for physical fitness, exerts significant stress on the spine , particularly due to prolonged hyperlordosis, postural stress and vascular risks . The paddling position, which involves excessive neck extension and sustained lumbar arching , can promote muscle tension and spinal dysfunction, and even lead to pathologies such as surfer’s myelopathy . Understanding these risks is essential to adopt prevention strategies and ensure surfing is safe for the spine.
Prolonged hyperlordosis: an underestimated risk factor
While paddling, surfers maintain prolonged hyperlordosis , that is, excessive arching of the lower back and neck, to keep the torso elevated and generate speed.
If this posture is held for too long, it can lead to:
- Increased compression of the spine , causing lower back pain and stiffness.
- Muscle tension in the cervical and thoracic region , promoting postural imbalances and contractures.
- Reduced blood flow to the spinal cord , increasing the risk of ischemia and neurological disorders.
Beginner surfers are particularly at risk because they spend more time paddling without the muscle strength to effectively support their spine .
Postural stress and its effect on the spine
In addition to the static posture of paddling, surfing places dynamic mechanical stress on the spine, due to rapid changes in position and constant adaptation to water movements.
- Neck and Thoracic Tension : Holding your head up for long periods can cause chronic neck pain and promote premature degeneration of the intervertebral discs.
- Lower back pain : Constant efforts to maintain balance put excessive strain on the stabilizing muscles of the trunk, which can lead to persistent back pain.
- Vertebral microtraumas : Repeated extension and flexion movements, combined with impacts with waves, can cause microscopic lesions of the intervertebral tissues, ultimately promoting pathologies such as herniated discs .
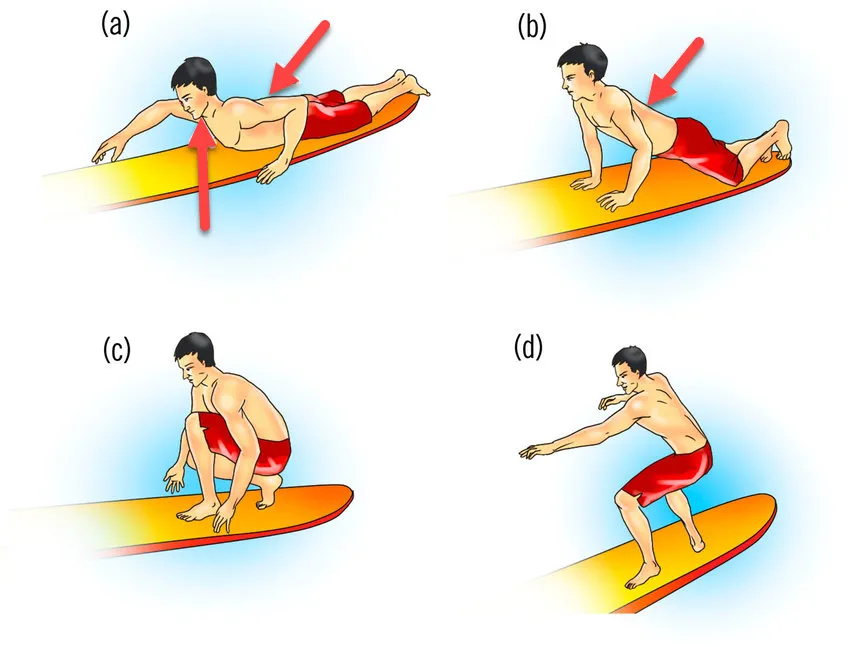
Additionally, sudden movements such as duck diving (diving under the wave) or pop-up (moving from a lying to standing position) impose sudden forces on the spine , increasing the risk of acute injuries.
Vascular risks associated with surfing
Beyond mechanical stress, surfing can also pose vascular risks to the spinal cord , due to prolonged compression and reduced blood flow.
- Slowing of venous return : Lying on the board for long periods can compress the inferior vena cava , causing blood stagnation and promoting circulatory disorders.
- Spinal cord ischemia : The hyperlordotic position can compress the anterior spinal artery , reducing oxygen supply to the spinal cord and causing neurological symptoms such as numbness or leg weakness.
- Effect of cold on blood circulation : Surfing in cold water can cause vasoconstriction , further limiting the irrigation of spinal structures and increasing the risk of ischemic lesions.
These mechanisms explain why surfer’s myelopathy is primarily caused by a combination of prolonged postural compression, ischemia, and repeated microtrauma .
Treatment and Rehabilitation Strategies
Management of surfer’s myelopathy is based on a multidisciplinary approach , aimed at reducing symptoms, restoring neuromuscular function and preventing recurrence. Appropriate treatment includes osteopathic approaches , targeted muscle strengthening , as well as pain relief techniques and management of long-term sequelae.
Osteopathic approaches and functional recovery
Osteopathy plays a vital role in the rehabilitation of patients suffering from surfer’s myelopathy, addressing muscle tension, joint blockages, and blood circulation. The primary goal is to rebalance the spine and promote optimal recovery of nerve and muscle structures.
- Myofascial release techniques : The osteopath works on accumulated tension in the cervical and thoracic region, thus reducing compression of nerve structures and improving mobility.
- Gentle spinal mobilization : Targeted manipulations help restore better force distribution on the spine and limit stress on the spinal cord.
- Improving spinal circulation : Through techniques aimed at promoting better vascular drainage, osteopathy helps to restore optimal blood flow to the spinal cord.
- Correction of postural imbalances : By readjusting the musculoskeletal structures, the osteopath helps prevent the reappearance of symptoms by optimizing the patient’s posture, particularly in rowing and surfing positions.
These approaches allow for progressive recovery by reducing pain and tension while improving flexibility and overall functionality of the spine.
Muscle strengthening and postural correction
Once the acute phase is under control, a muscle rehabilitation program is essential to restore strength and stability to the spine. The goal is to strengthen the stabilizing muscles , while working on flexibility and coordination.
- Core training : Specific exercises (plank, dynamic core training, Pilates) strengthen the abdominal muscles and limit excessive stress on the spine.
- Cervical and thoracic mobility work : Controlled range of motion exercises help restore joint flexibility while reducing the risk of spinal cord overcompression.
- Correcting posture on the board : Learning a better paddling position and standing transition helps avoid overloading the cervical and lumbar vertebrae.
- Targeted stretches : Stretching the hip flexors, lower back muscles, and shoulders helps prevent excessive tension that promotes the onset of myelopathy.
Incorporating these exercises into a regular routine is essential to prevent recurrence and allow a safe return to surfing.
Pain relief techniques and after-effect management
Depending on the severity of the myelopathy, residual pain or neuromuscular disorders may persist. Comprehensive management of pain and after-effects is based on several strategies:
- Physiotherapy and neuromotor rehabilitation : In addition to strengthening exercises, rehabilitation techniques help to regain optimal coordination and proprioception .
- Manual therapy and therapeutic massages : These interventions help reduce muscle tension and residual pain , while promoting tissue recovery.
- Neurostimulation techniques : In some cases, the use of electrostimulation or neuromodulation techniques may be considered to reactivate certain nerve functions and reduce pain.
- Alternative approaches : Meditation, deep breathing, and yoga are useful tools for improving stress management, which can increase muscle tension and pain perception.
Prevention: How to Reduce Risks?
Surfer’s myelopathy is a condition that can be avoided by adopting preventative habits aimed at limiting spinal cord compression and optimizing the surfer’s posture and physical condition. Three main areas are essential to reducing risks : improving posture on the board, incorporating specific exercises, and intelligently managing the intensity of the practice.
Adopt an optimal posture on the board
The paddling position is one of the key factors in the occurrence of surfer’s myelopathy, as it imposes prolonged hyperextension of the cervical and thoracic spine . Adjusting this posture can significantly reduce the stress placed on the spinal cord.
- Avoid excessive neck extension : It is recommended to keep the head in line with the trunk rather than raising it excessively, which reduces compression of the cervical structures.
- Use your back and trunk muscles : Engaging your core muscles (abdominals, lumbar, back) helps distribute the load better and avoid overloading the cervical vertebrae.
- Do not over-arch the lower back : Excessive lordosis can be minimized by activating the abdominals and finding a balance between mobility and stability .
- Alternate resting positions : Take short breaks between rowing sessions to release tension on the spine and allow better vascularization of the spinal cord.
Adopting a more ergonomic and dynamic posture on the board can not only prevent myelopathy , but also improve surfers’ performance and endurance.
Targeted exercises and stretches for surfers
A proper training program can help prepare the spine for the stresses of surfing and minimize the risk of injury. Emphasis should be placed on strengthening stabilizer muscles , improving flexibility and spinal mobility.
Muscle strengthening exercises
- Core strengthening : Dynamic core exercises (plank, hollow body hold, bird-dog) help improve spinal stability.
- Postural muscle work : Back extensions (Superman, reverse planks) strengthen the erector spinae muscles, better supporting the rowing posture.
- Shoulder Strengthening : External rotations and resistance band exercises promote better shoulder muscular endurance for rowing.
Spinal Stretching and Mobility
- Hip flexor and lower back stretch : Couch stretch and cobra pose (yoga) help release lower back tension.
- Cervical mobilization : Gentle flexion-extension and rotation movements of the neck help prevent stiffness.
- Stretching the thoracic and scapular muscles : Use a foam roller on the thoracic spine to improve the opening of the bust and relieve tension.
Incorporating these exercises into a regular routine improves resistance to the mechanical stresses of surfing and decreases the likelihood of prolonged spinal cord compression.
Recovery time and adjustment of practice intensity
One of the aggravating factors of surfer’s myelopathy is excessive time spent in the paddling position, combined with a lack of recovery. Intelligent management of surfing sessions and rest time is essential to prevent spinal cord disorders.
Managing cold exposure : Cold water surfing can aggravate vasoconstriction and vascular compression. Adequate warm-up and the use of appropriate thermal wetsuits can minimize these effects.
Limit the duration of prolonged rowing sessions : Alternating between rowing phases and periods of rest on the board (sitting or lying on your side) helps reduce the load on the cervical and thoracic spine.
Respect the body’s warning signals : If tingling, a feeling of heavy legs or muscle weakness appears, it is crucial to immediately interrupt the session and rest.
Progress gradually : For beginners, it is recommended to gradually increase the intensity and duration of sessions, avoiding excessive efforts over long periods from the start.
Promote active recovery : After an intense session, incorporate mobility, hydration and active recovery exercises (yoga, gentle swimming) to promote better blood circulation.
Key steps to avoid surfer’s myelopathy
1. Education on Technique and Posture
Proper education on paddling and posture is fundamental in preventing spinal stress and reducing the likelihood of developing surfer’s myelopathy. Maintaining a neutral spinal alignment while paddling and transitioning to standing can help minimize excessive pressure on the spinal cord.
- Avoid excessive hyperextension of the lower back and neck. Keep the head in a natural position rather than constantly looking forward, which increases cervical compression.
- Engage core and back muscles. Proper engagement of the core and lower back muscles helps distribute the effort, reducing strain on the spine.
- Modify paddling position periodically. Alternating positions, such as shifting weight slightly or taking short breaks by sitting on the board, can help reduce sustained stress on the spine.
- Ensure a controlled and smooth transition from paddling to standing. Avoid jerky movements that place excessive strain on the lower back.
2. Strengthening and Flexibility Training
A well-designed exercise routine can significantly reduce the risk of developing surfer’s myelopathy by improving spinal stability and flexibility.
- Core and lower back strengthening: Strengthening the core (planks, bird-dogs, bridges) enhances spinal support and prevents excessive spinal extension during paddling.
- Neck and upper back exercises: Strengthening the cervical muscles (chin tucks, isometric neck exercises) reduces the risk of excessive compression in the neck region.
- Flexibility training: Stretching the hip flexors, hamstrings, and spinal extensors can help maintain a healthy posture and reduce stiffness.
- Thoracic spine mobility exercises: Using a foam roller or performing mobility drills can improve spinal flexibility and reduce tension.
3. Use of Protective Equipment
Certain protective gear can provide added spinal support and help prevent excessive strain during prolonged surfing sessions.
- Wearing a flotation vest: Properly fitted flotation devices can reduce the load on the spine by promoting a more buoyant position while paddling.
- Using ergonomic surfboard designs: Boards with more buoyancy can help maintain a more comfortable paddling position, reducing excessive back arching.
- Considering neoprene or lumbar support gear: Some surfers find additional support from compression garments that help stabilize the lower back and core muscles.
4. Managing Surfing Sessions: Rest and Recovery
Limiting prolonged exposure to the hyperextended position and allowing adequate recovery are essential components of injury prevention.
- Take regular breaks. Every 15-20 minutes, take a short break by sitting on the board or stretching to relieve spinal stress.
- Listen to your body. If numbness, tingling, or weakness begins to develop, stop surfing immediately and allow for rest and recovery.
- Manage exposure to cold water. Surfing in cold conditions can contribute to vasoconstriction, further limiting spinal blood flow and increasing the risk of ischemia. Wearing adequate wetsuits to maintain warmth can help prevent vascular complications.
- Increase session intensity gradually. Novice surfers should start with shorter sessions and progressively build endurance rather than engaging in prolonged paddling early on.
5. Post-Surf Recovery and Monitoring
Recovery plays a crucial role in spinal health, particularly after prolonged paddling sessions. Post-surf rehabilitation techniques can help prevent long-term complications.
Hydration and circulation: Proper hydration supports optimal circulation, which is crucial in preventing ischemic conditions affecting the spinal cord.
Stretching routine: Focus on lumbar and cervical decompression stretches, such as the cat-cow stretch, child’s pose, and thoracic extensions, to relieve spinal stress.
Foam rolling and massage therapy: Using self-myofascial release techniques can alleviate muscular tension in the lower back, shoulders, and neck.
Long-Term Prognosis and Outlook
The prognosis for surfer’s myelopathy varies depending on the severity of the neurological damage, the speed of diagnosis, and the implementation of appropriate treatment. While some surfers recover completely after a few weeks or months, others may have more or less severe after-effects. Understanding the factors influencing recovery , the possibilities for returning to surfing , and strategies to avoid recurrence is essential to support patients towards optimal rehabilitation.
Factors influencing recovery
Recovery from surfer’s myelopathy depends on several factors:
1. Severity of initial lesions
- Mild to moderate forms (numbness, partial muscle weakness) have a favorable prognosis, with gradual recovery over a few weeks to a few months .
- Severe cases , involving complete paralysis or sphincter disorders , may require longer rehabilitation, and recovery may be partial.
2. Speed of diagnosis and treatment
- Early medical intervention ( immediate rest, appropriate therapies) improves the prognosis by preventing the worsening of lesions.
- Delayed diagnosis can lead to irreversible spinal cord damage and persistent deficits.
3. Nerve regeneration capacity
- The spinal cord has a limited capacity for regeneration after prolonged ischemia or compression. Recovery is therefore more uncertain in cases of prolonged nerve fiber damage.
- Multidisciplinary care ( osteopathy, physiotherapy, muscle strengthening) is essential to stimulate functional recovery .
4. Patient engagement in rehabilitation
- An adapted rehabilitation program (strengthening, mobilization, postural correction) accelerates recovery and reduces the risk of recurrence.
- Returning to surfing too early without adapting technical gestures can aggravate symptoms and compromise the healing process.
Can you surf after myelopathy?
The question of returning to surfing after myelopathy depends on individual recovery and adjustments made to prevent recurrence.
1. In what cases is a return possible?
- If motor and sensory function is restored , a gradual return can be considered after medical agreement .
- Patients who have fully recovered without after-effects can resume surfing , subject to specific precautions .
- Those with mild after-effects (residual numbness, moderate weakness) should adapt their practice and avoid sessions that are too long.
2. When should you avoid resuming?
- If motor or sensory deficits persist, making coordination difficult.
- In case of chronic pain or recurring cervical tension which risks being reactivated with the rowing posture.
- If neurological symptoms reappear quickly after resuming practice.
3. How to resume safely?
- Gradually , by limiting the duration of sessions and avoiding excessive rowing.
- By working on posture , particularly by adjusting the rowing position to reduce cervical hyperextension.
- By incorporating warm-ups and cool-down exercises after each session.
Resuming surfing is possible in many cases, but it requires medical monitoring and adaptation of technique to avoid reproducing the conditions that led to the pathology.
Adapt your practice to prevent recurrences
Surfers who have suffered from myelopathy must absolutely modify certain aspects of their practice to avoid further spinal cord damage.
1. Optimizing rowing posture
- Reduce cervical hyperextension by aligning the neck with the trunk instead of raising it too high.
- Regularly mobilize the spine by alternating positions (sitting, lying on the side) during breaks.
- Engage the core muscles to distribute the effort and limit the overload on the neck.
2. Strengthening and mobility work
- Strengthen the abdominal and back strap to support the spine.
- Improve cervical and thoracic flexibility through specific stretching exercises.
- Practice yoga or Pilates to strengthen the body without excessive stress on the spine.
3. Practice time management and recovery
- Avoid prolonged sessions , especially after a period of inactivity.
- Schedule regular breaks to relieve stress on the spine and stimulate blood circulation.
- Recover well after each session by incorporating muscle relaxation techniques (massage, osteopathy, hydrotherapy).
4. Symptom monitoring and medical prevention
- Stay alert for the first signs of numbness or muscle fatigue.
- Consult an osteopath or physiotherapist regularly to ensure that your posture and technical movements are appropriate.
- Do not hesitate to modify the frequency and intensity of the sessions depending on the evolution of your health.
Long-Term Prognosis
The long-term prognosis for surfer’s myelopathy depends on the severity of spinal cord damage and how quickly diagnosis and treatment are initiated. In cases where the condition is detected early and treated appropriately, patients can expect significant recovery, although this may take several months or even years. However, some patients may continue to experience residual symptoms, such as muscle weakness, numbness, or coordination problems, which may affect their ability to engage in surfing or other intensive physical activities. The risk of recurrence is also an important consideration, especially if necessary modifications to surfing technique or posture are not implemented. It is essential that patients follow a rigorous rehabilitation program and make a long-term commitment to maintaining good physical condition to avoid relapses. In more severe cases, where nerve damage is extensive, the prognosis may be poorer, with an increased risk of permanent neurological deficits.
Conclusion
Surfer’s myelopathy, although rare, poses a serious threat to surfers, particularly novices who spend long periods hyperextended on their boards. This condition perfectly illustrates the impact that prolonged postural constraints can have on the spine and spinal cord. Its delayed diagnosis often complicates treatment, highlighting the importance of increasing awareness among surfers and healthcare professionals.
In the face of this risk, prevention plays a central role. Adopting optimized rowing techniques, targeted muscle strengthening, and properly managing recovery times are all measures that can minimize the incidence of this condition. In addition, osteopathy and specialized rehabilitation offer effective solutions to promote recovery and prevent recurrence.
While surfing is synonymous with fun and freedom, it shouldn’t come at the expense of spinal health. By incorporating appropriate strategies and paying attention to your body’s signals, you can continue to enjoy the waves while protecting your spine. A well-thought-out preventative approach allows you to combine passion and safety, ensuring surfers have a more sustainable and safe experience.
References
- Thompson TP, Pearce J, Chang G, Madamba J.. Surfer’s myelopathy. Spine (Phila Pa 1976). 2004;29(16):E353–6. doi: 10.1097/01.BRS.0000134689.84162.E7 [PubMed] [CrossRef] [Google Scholar]
- Nathanson A, Bird S, Dao L, Tam-Sing K.. Competitive surfing injuries: a prospective study of surfing-related injuries among contest surfers. Am J Sports Med. 2007;35(1):113–7. doi: 10.1177/0363546506293702 [PubMed] [CrossRef] [Google Scholar]
- Nathanson A, Haynes P, Galanis D. Surfing injuries. Am J Emerg Med 2002;20(3):155–60. doi: 10.1053/jem.2002.32650 [ PubMed ] [ CrossRef ] [ Google Scholar
- Wadia S, Padmanabhan P, Moeller K, Rominger A.. Pediatric surfer’s myelopathy. J Emerg Med. 2015;49(5):e143–5. doi: 10.1016/j.jemermed.2015.06.065 [PubMed] [CrossRef] [Google Scholar]
- Conidi F. Some unusual sports-related neurologic conditions. Continuum (Minneap Minn). 2014;20(6 Sports Neurology):1645–56. [PubMed] [Google Scholar]
- Maharaj MM, Phan K, Hariswamy S, Rao PJ.. Surfer’s myelopathy: a rare presentation in a non-surfing setting and review of the literature. J Spine Surg. 2016;2(3):222–6. doi: 10.21037/jss.2016.09.07 [PMC free article] [PubMed] [CrossRef] [Google Scholar]
- Freedman BA, Malone DG, Rasmussen PA, Cage JM, Benzel EC.. Surfer’s myelopathy: a rare form of spinal cord infarction in novice surfers: a systematic review. Neurosurgery. 2016;78(5):602–11. doi: 10.1227/NEU.0000000000001089 [PubMed] [CrossRef] [Google Scholar]
- Nakamoto BK, Siu AM, Hashiba KA, Sinclair BT, Baker BJ, Gerber MS, et al. Surfer’s myelopathy: a radiologic study of 23 cases. AJNR Am J Neuroradiol. 2013;34(12):2393–8. doi: 10.3174/ajnr.A3599 [PMC free article] [PubMed] [CrossRef] [Google Scholar]
- Robles LA. Letter: surfer’s myelopathy: a rare form of spinal cord infarction in novice surfers: a systematic review. Neurosurgery. 2017;80(6):E266. doi: 10.1093/neuros/nyx044 [PubMed] [CrossRef] [Google Scholar]
- Takakura T, Yokoyama O, Sakuma F, Itoh R, Romero RR.. Complete paraplegia resulting from surfer’s myelopathy. Am J Phys Med Rehabil. 2013;92(9):833–7. doi: 10.1097/PHM.0b013e3182411f58 [PubMed] [CrossRef] [Google Scholar]
- Nathanson AT. Surfing injuries. In: Mei-Dan O, Carmont MR, (eds.) Adventure and Extreme Sports Injuries: Epidemiology, Treatment, Rehabilitation and Prevention. London: Springer; 2013. p. 143–72. [Google Scholar]
- Aoki M, Moriizumi S, Toki M, Murakami T, Ishiai S.. Rehabilitation and long-term course of nontraumatic myelopathy associated with surfing. Am J Phys Med Rehabil. 2013;92(9):828–32. doi: 10.1097/PHM.0b013e318238a1d0 [PubMed] [CrossRef] [Google Scholar]
- Sunshine S. Surfing injuries. Curr Sports Med Rep. 2003;2(3):136–41. doi: 10.1249/00149619-200306000-00005 [PubMed] [CrossRef] [Google Scholar]
- Renneker M. Surfing: the sport and the life-style. Phys Sportsmed. 1987;15(10):156–62. doi: 10.1080/00913847.1987.11702109 [CrossRef] [Google Scholar]
- Moeller JL, Rifat SF.. Spondylolysis in active adolescents: expediting return to play. Phys Sportsmed. 2001;29(12):27–32. doi: 10.3810/psm.2001.12.1074 [PubMed] [CrossRef] [Google Scholar]
- Aviles-Hernandez I, Garcia-Zozaya I, DeVillasante JM.. Nontraumatic myelopathy associated with surfing. J Spinal Cord Med. 2007;30(3):288–93. doi: 10.1080/10790268.2007.11753939 [PMC free article] [PubMed] [CrossRef] [Google Scholar]
- Chung HY, Sun SF, Wang JL, Lai PH, Hwang CW.. Non-traumatic anterior spinal cord infarction in a novice surfer: a case report. J Neurol Sci. 2011;302(1–2):118–20. doi: 10.1016/j.jns.2010.11.026 [PubMed] [CrossRef] [Google Scholar]
- Albuja AC, Qaiser S, Lightner DD, Raslau FD, Zafar MS, Bernard PA, et al.. Surfer’s myelopathy without surfing: a report of two pediatric patients. Spinal Cord Ser Cases. 2017;3:17008. doi: 10.1038/scsandc.2017.8 [PMC free article] [PubMed] [CrossRef] [Google Scholar]
- eixeira S, Moser F, Kotton RH.. Imaging features and differentials in surfer’s myelopathy: a case report. Emerg Radiol. 2016;23(1):89–92. doi: 10.1007/s10140-015-1346-1 [PubMed] [CrossRef] [Google Scholar]
- Choi J, Seok HY, Kim Y, Kim BJ.. Surfer’s myelopathy mimicking infectious myelitis. J Clin Neurol. 2017;13(2):207–8. doi: 10.3988/jcn.2017.13.2.207 [PMC free article] [PubMed] [CrossRef] [Google Scholar]
- Scatchard R, Alves Rosa J, Bowen P, Mortimer A, Sharples PM, Lux AL.. A case report: paediatric surfer’s myelopathy. Eur J Paediatr Neurol. 2018;22(1):199–202. doi: 10.1016/j.ejpn.2017.09.011 [PubMed] [CrossRef] [Google Scholar]
- Sugiyama N, Yokoyama JI, Ikegami M, Matsuda S, Miyashita Y. A child case of surfer’s myelopathy. No To Hattatsu . 2016;48(1):41–4. [ PubMed ] [ Google Scholar ]